Healthcare for all in India: When, How, and Why RSBY?
- Essential Services
- by Oommen C Kurian
- 27 Jul, 2015
Sharelines
 Free quality public services are vital to fight poverty and inequality by putting virtual money in people’s pockets.http://bit.ly/1Ipuoeb
Free quality public services are vital to fight poverty and inequality by putting virtual money in people’s pockets.http://bit.ly/1Ipuoeb
 Every year, health payments push 6 crore Indians below poverty line. Know more. http://bit.ly/1Ipuoeb
Every year, health payments push 6 crore Indians below poverty line. Know more. http://bit.ly/1Ipuoeb
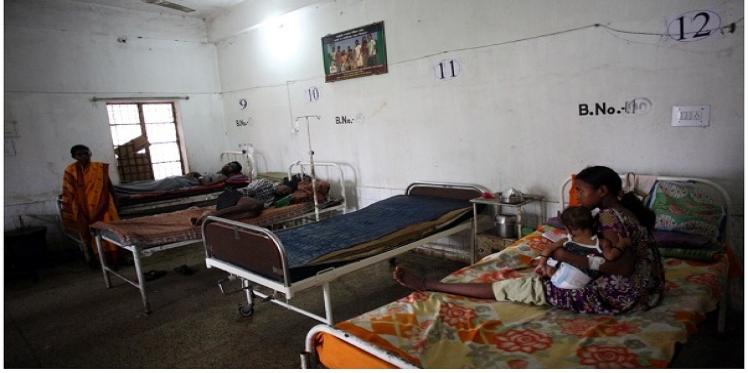
India’s health system is one of those rarities in international health where enthusiastic policy discourse on Universal Health Coverage (UHC) and user charges co-exist. On the one hand, India has plans around health tourism focusing on super-specialty hospitals in the cities; on the other, every year, health payments push 60 million Indians (6 crore) below poverty line.
India’s overall public spending hovers at about 1% of GDP while corresponding figures are much higher for Brazil (4.5%) and United Kingdom (8%). In this regard, spending cuts on public services by the central budget of 2015-16 are deeply concerning. A recent paper brought out by Oxfam India explored available evidence around financing healthcare for all in India and offered recommendations.
Owing to devastating effects of catastrophic out of pocket (OOP) spending, it became politically untenable to continue pushing policy options like user charges, and UHC was seen as a solution. In a way, for many international institutions like the World Bank and experts like David de Ferranti, the promotion of UHC often meant a reversal of some of their previously held policy positions.
In an interview just before its biannual meeting in 2014, the World Bank head Jim Yong Kim admitted: “There’s now just overwhelming evidence that those user fees actually worsened health outcomes. There’s no question about it. So did the bank get it wrong before? Yeah. I think the bank was ideological”.
This echoed the words of the WHO head, Margaret Chan from five years ago: “User fees for healthcare were put forward as a way to recover costs and discourage the excessive use of health services and the over-consumption of care. This did not happen. Instead, user fees punished the poor”.
The recent Lancet Commission on Investing in Health focused on public financing mechanisms and redistributive risk pools in reaching UHC. Yates and Dhillon (2014) observe that the commission also explicitly rejected the 1993 World Development Report’s (WDR) emphasis on private financing including user fees. This marks a new consensus.
Unfortunately, this new consensus has not yet had much policy impact in India. Indian public healthcare delivery system still has user charges, and exemptions and waivers are known to be extremely ineffective. Indian public health system is also being pushed towards an insurance-based model, which will be more private sector friendly, based on the experience with Rashtriya Swasthya Bima Yojana (RSBY), an insurance scheme targeting the below poverty line households.
Despite the inconclusive and generally negative evidence, the high praise given to RSBY and other health insurance schemes by influential agencies including the World Bank Group and the International Labour Organisation (ILO) has contributed significantly to its policy popularity. An Oxfam paper published in 2013 termed such praise as “both premature and dangerously misleading”.
Influence of World Bank Group on the Indian Health System: Equity and Lending
An interesting aspect of private sector expansion in India – along with government largesse and subsidies- is the nature of funds that many private hospital chains attract. The World Bank Group’s commitment to universal and equitable health coverage and to shared prosperity, while welcome, is often at odds with its investment priorities. In India, the International Finance Corporation (IFC) has aided corporate expansion into the hospital sector through loans and advice to the private sector.
Research by Oxfam in 2014 has shown that all the members of the World Bank Group are not aligned in its objectives of UHC and equity in health. To cite from Africa’s experience, the research finds a failure to analyse how to reach poor people effectively via the private sector, failure to direct investments for the benefit of poor people, and failure to even measure whether poor people are being reached.
Indian private healthcare sector represents more than 30 % of IFC’s global healthcare investment portfolio. However, the role and impact of loan recipients on the health system- as in the case of Africa- remains questionable and needs further research to understand this better. Oxfam India’s Working Paper reveals that many recipients of IFC loans in India are major flouters of existing legal requirements mandating access to poor patients.
Skimming through the limited investment information available on the IFC website, we find that four hospitals in New Delhi alone failed to meet their legal obligations to deliver a certain percentage of their services to the underserved, received around $320 million (around Rs 2000 crore at current exchange rates) over the last decade. This is about 10% of the total plan outlay for health in India’s 2015-16 budget.
Evidence-based Policymaking?
Thus, it is in the context of an aggressively expanding private healthcare sector that promotion of insurance schemes to channelize tax money to the private sector must be looked at. It is clear from available evidence that there is no objective basis to claims that insurance based models should be the vehicle for India’s efforts towards UHC.
In this regard, it is observed that there is resistance to objectively evaluate government-funded insurance schemes. Fan and Mahal (2011) note that politicians and administrators often presume that independent evaluations are more damaging than beneficial. Moreover, state governments in India are also known to be hesitant to conducting independent evaluations of health insurance schemes, and RSBY, where it is often claimed that some “rigorous assessment” of its impact is done, admittedly shares its scheme data “only with a carefully selected group of researchers”.
This damning observation was made four years ago in an editorial of a leading medical journal of India, but the situation has not changed much. Added to this, disaggregated data on reimbursements to public hospitals and private hospitals remain unavailable in the public domain.
Interestingly, after RSBY came into the spotlight as a successful international UHC case study and seen as a potential model to expedite India’s efforts towards healthcare for all, the RSBY data portal discontinued uploading even the basic state level data that used to be infrequently updated earlier.
The latest data available on the portal is from the first quarter of 2014. The latest evaluation on the portal is from the first quarter of 2013. For states like Bihar, latest data from many districts are from 2012.
To compound this, the allegation that RSBY is a private sector subsidy scheme remains, particularly in the light of high prevalence of corruption and the limited, or even negative, impact that the scheme seems to have on checking OOP spending. If RSBY becomes the foundation of India’s efforts towards UHC, it will have long-term negative implications to the health system.
Instead of relying on an insurance-based financing model, it is proven that effective tax-financing of public services is a cornerstone of a well-functioning democracy.
Results of recently-conducted cross-national modelling in 89 low-income and middle-income countries show that each Rs10 per capita increase in tax revenue resulted in an additional Rs1 of public health spending per capita while a Rs10 increase in GDP per capita resulted in an increase of Rs 0.10.
Health experts in India have come out in open support of public infrastructure improvement and against insurance-based solutions. They warn about the dangers of India moving towards a system of lightly-regulated health insurance coverage, as the task of regulating the system can be “beyond daunting”, and it is far easier for the government to improve the functioning of health services that are directly under its control.
Needless to add, how the mobilised tax resources are spent despite the budgetary constraints and implementation bottlenecks is as important as expanding the base in the context of progressive taxation. Free quality public services are vital to fight poverty and inequality by putting virtual money in people’s pockets, and, as Oxfam research from 2014 has shown, do the opposite of what user charges do.
In the light of the Third International Financing for Development Conference rejecting the call for a global tax body, it is time to step up civil society advocacy to make tax systems more equitable and efficient in order to support stronger public services, including healthcare for all.
Written by: Oommen C Kurian, Research Coordinator, Oxfam India
Photo Credit: Srikanth Kolari
Essential Services
We focus on ensuring access to quality and affordable health and education for all
Read MoreRecent Blogs
Making Sanitation & Hygiene Facilities Accessible—Delhi Flood Response
Aug 4, 2023 | Savvy
Psychosocial Counselling for Balasore Train Tragedy Survivors
Jul 6, 2023 | Savvy
The Oxfam India Legacy Will Live On
May 30, 2023 | Savvy
Inequality In Parliament
Mar 31, 2023 | Savvy
International Women's Day Round Up
Mar 30, 2023 | Savvy
Why Women in India Earn Less And Get Fewer Jobs—Discrimination
Mar 2, 2023 | Savvy
The Inequality Issue
Jan 17, 2023 | Savvy
Oxfam India in 2022: 10 People 10 Stories
Mar 9, 2023 | Savvy
Boosting the Rural Economy | Parab Festival
Dec 23, 2022 | Savvy
Striving for Financial Inclusion: Need Women-Friendly Ecosystem
Dec 2, 2022 | Savvy
Primary Prevention of Violence Against Women and Girls And the Role of Civil Society Organisations
Nov 28, 2022 |
Bottom Up Approach: Strengthening School Management Committees For Better Schools
Nov 22, 2022 | Savvy
Disconnecting 1098 Is A Bad Idea
Nov 14, 2022 | Savvy
11 Facts About Education In India That You Need To Know
Oct 31, 2022 | mahika@oxfamindia.org
Assam Floods | Our Response Updates
Oct 3, 2022 | Savvy
India Discrimination Report | 8 Things You Need To Know
Sep 15, 2022 | Savvy
For The Youth To Rise Against Inequality, We Must Work With Them
Aug 12, 2022 | Savvy
The Consequences of School Closures on Adivasi Children
Aug 9, 2022 | Savvy
Celebration of Iconic Days In Mohalla Classes
Jun 29, 2022 | Savvy
Financial Literacy Awareness Continues
Jun 29, 2022 | Savvy
I Want To Join The Army
May 30, 2022 | Savvy
Financial Literacy Camps For Women Farmers
May 30, 2022 | Savvy
Education Opens The Doors Of Freedom, Yet Again
May 5, 2022 | Savvy
Bitter Sugar: Cane Cutters Charter of Demands
May 26, 2022 | Savvy
International Women's Day | The Week That Was
Mar 21, 2022 | Savvy
Building A Responsible Sugar Supply Chain
Feb 20, 2022 | Savvy
Empowerment Not Age: Examining The Complexities Of Child, Early And Forced Marriages
Feb 16, 2022 | Savvy
Dominance by Billionaires Leads India’s Highway to Record Levels of Inequality
Jan 25, 2022 | Savvy
Why We Need To Stand Up For The Cane Cutters
Jan 13, 2022 | Savvy
फ़ातिमा शेख़: देश की पहली मुस्लिम शिक्षिका को नमन
Jan 9, 2022 | Savvy
2021: Your Journey With Oxfam India
Dec 31, 2021 | Savvy
Policing Adolescent Sexuality And Health Consequences
Jan 17, 2022 | Savvy
16 Days of Activism
Dec 17, 2021 | admin
Women's Land Rights Are Human Rights
Dec 16, 2021 | Savvy
A Child-Friendly Environment Is Essential To Children's Rights
Dec 14, 2021 | Savvy
Urban Food Hive Project: Nourish The Cities
Feb 28, 2022 | Savvy
महिलाओं को मिले बराबरी का हक तो बदल सकती है खेती-किसानी की सूरत
Oct 15, 2021 | Savvy
Only Together… Can We Save Our Rivers!
Oct 12, 2021 | Savvy
Chhattisgarh Roundtable: Implementation of PWDVA
Oct 10, 2021 | Savvy
Multi-Stakeholder Consultation on Fisheries Management
Oct 10, 2021 | Savvy
What Sugarcane Farmers Want
Oct 8, 2021 | Savvy
How Unequal is Inequality?
Oct 6, 2021 | Savvy
Bring Teachers To School: UP’s Unfilled Vacancies and Its Impact
Oct 4, 2021 | Savvy
The Case of Low Conviction in Crimes Against Dalits and Adivasis
Sep 29, 2021 | Savvy
शिक्षा से वंचित बच्चों को विद्यालय में लाने की मुहीम
Oct 10, 2021 | Savvy
Initiating Work With Cane Cutters in Maharashtra
Sep 16, 2021 | Savvy
शिक्षक दिवस पर सावित्री बाई फुले को श्रद्धांजलि
Sep 5, 2021 | Savvy
Questions On Healthcare, Education And Inequality Raised In Parliament
Sep 1, 2021 | Savvy
ट्रोसा परियोजना के क्रियान्वयन से जागरूक हुआ ग्रामीण समुदाय
Sep 15, 2021 | Savvy
Oxfam India Pushes for Implementation of Patients’ Rights Charter
Aug 7, 2021 | Savvy
Cyclones, Flood, and COVID-19 Upends Lives in Odisha’s Soro Block
Jul 23, 2021 | Savvy
SDG Index: A Long Way To Go
Jul 7, 2021 | Savvy
Our Women Water Champions
Jun 4, 2021 | Savvy
COVID-19 in Assam’s Tea Gardens
May 17, 2021 | Savvy
Informal Sector Workers In A Policy Blind Spot
Jun 7, 2021 | Savvy
Positive Gender Social Norms For A Better Society
Apr 15, 2021 | Savvy
From Conflict to Cooperation
Apr 9, 2021 | Savvy
Oxfam India journey to end discrimination – glimpses from 2020
Apr 1, 2021 | Anisha
Oxfam India's International Women’s Day Celebrations
Mar 14, 2021 | Savvy
Forest Rights Recognised In Jharkhand for the First Time in Two Years
Mar 12, 2021 | Savvy
छत्तीसगढ़ बजट 2021: वनाधिकार के नजरिये से
Mar 2, 2021 | Savvy
Transforming Lives Of Tribal Women With Energy Efficient Cook-Stoves
Feb 19, 2021 | Savvy
The Inequality Virus Released in States
Feb 14, 2021 | Savvy
Implementing Patients’ Rights Charter: Step towards Accessible Health
Jan 12, 2021 | Savvy
To Be or Not To Be: Minimum Age of Marriage for Girls
Jan 12, 2021 | Savvy
Addressing Early Marriages in India (Oxfam India-SAWM Webinar)
Dec 23, 2020 | Savvy
The Right Age for Marriage: Should the State Decide?
Dec 3, 2020 | Savvy
#EmpowermentNotAge
Jan 4, 2021 | radhika
#EmpowermentNotAge
Apr 1, 2021 | radhika
5 Reasons Changing The Minimum Age Of Marriage Is A Bad Move
Dec 23, 2020 | radhika
The Status of Implementation of PWDVA: Odisha Consultation
Sep 30, 2020 | Savvy
Right To Property: An Imperative For Freedom
Sep 30, 2020 | Savvy
A Salute to the Architects of Our Society
Sep 30, 2020 | Savvy
शारदा नदी बेसिन में सिंचाई की पद्धतियों पर एक अनुभव
Sep 30, 2020 | Savvy
Chhattisgarh Recognises CFR Rights – A First Since FRA’s inception
Aug 25, 2020 | Savvy
Legal Reforms to Increase Age of Motherhood — Will It Work?
Sep 30, 2020 | radhika
समानता के सिद्धान्त को आदिवासी सिखलाता है
Aug 9, 2020 | Savvy
The Need to Uphold RTE Act During a Pandemic
Aug 5, 2020 | Savvy
My Internship Experience at Oxfam India
Aug 21, 2020 | radhika
Comprehensive Regulatory Framework for Private Schools Needed
Aug 4, 2020 | Savvy
Measures to Increase Reporting of Domestic Violence, a Parallel Pandemic
Sep 30, 2020 | radhika
Locked-down: Domestic Violence Reporting in India during COVID-19
Sep 30, 2020 | radhika
Agriculture & COVID-19: Pro Women Farmer Policies Needed
Aug 1, 2020 | Savvy
The Loot of Private Healthcare
Jul 17, 2020 | Savvy
Protecting Children's Rights during Lockdown
Jul 15, 2020 | Savvy
The SWaCH Story | How waste pickers continued work during lockdown
Mar 5, 2021 | Savvy
Inclusive Economic Opportunities for Brahmaputra River Communities
Jun 30, 2020 | Savvy
How can India’s education system escape the vicious cycle of inequality and discrimination?
Jun 30, 2020 | radhika
Haq Se… We (He, She and Ze) are all Equal!
Jun 30, 2020 | Savvy
Living the Rainbow Dream
Jun 30, 2020 | Savvy
Tea Workers in a Tough Spot
Jun 30, 2020 |
Mental Health In COVID-19
Jun 30, 2020 | radhika
Milk for the Twins
Jun 24, 2020 |
The COVID-19 Impact on Waste Pickers in Delhi
Jun 24, 2020 |
Yes, It is That Time of the Month!
Jun 30, 2020 |
It is Raja Festival, Let’s Talk about Periods
Jun 15, 2021 |
पर्यावरण बचाना होगा
Jun 30, 2020 | Savvy
COVID-19 Is Covering For Nature, Are We?
Jun 30, 2020 | radhika
Cyclone Amphan’s Trail of Devastation
Jul 29, 2020 | Savvy
COVID-19 Pandemic: Oxfam India is Responding
May 31, 2020 | Savvy
Oxfam India Prepares Ahead of Cyclone Amphan Landfall
Jul 29, 2020 | Savvy
On Foot, On Truck and Finally, A Bus
May 31, 2020 | Savvy
Getting Home, Somehow
May 31, 2020 | Savvy
COVID Lockdown Makes Meeting Ends Difficult
May 31, 2020 | Savvy
A Bleak Future
May 28, 2020 | Savvy
A virus that exploits racism
May 31, 2020 | radhika
COVID-19 Reveals Deep Vulnerabilities in India’s Labour
May 31, 2020 |
COVID-19 CSR Appeal By Oxfam India
May 31, 2020 | radhika
Recognising land rights this International Day of Forests
May 31, 2020 | radhika
Covid Cooperation: United We Survive
May 31, 2020 | Animesh Prakash
Coronavirus and Inequality
May 31, 2020 | radhika
Government of Odisha releases Climate Budget 2020-2021
May 31, 2020 | radhika
Feminism through Movies at the Raipur film festival
Jun 3, 2020 | radhika
How Oxfam India Transformed Lives in 2019
Jun 3, 2020 | Anisha
The Story Behind Beyond Charity (Oxfam India's 10 Year Journey)
Jun 3, 2020 | radhika
Rapid Needs Assessment for Unprecedented Floods in Uttar Pradesh
Jun 3, 2020 | radhika
Access to energy for livelihood security
Dec 5, 2019 | radhika
Truth About Tea Campaign at Lucknow's Kabir Festival
Jun 3, 2020 | radhika
Reflections from UN Forum on Business and Human Rights 2019
Dec 18, 2019 | radhika
State Consultation Meeting on Forest Rights Act 2006
Dec 5, 2019 | radhika
Say yes to #EqualWaliDiwali
Dec 5, 2019 | radhika
Do a Good Deed and Save Tax
Oct 23, 2019 | Anisha
Youth spearhead the #CleanPatnaDrive in Bihar
Dec 5, 2019 | radhika
Celebrate Daan Utsav with Oxfam India
Oct 9, 2019 | radhika
Forest rights leading to livelihood security
Oct 9, 2019 | radhika
Love is always violence free
Dec 5, 2019 | radhika
Long wait, delayed returns
Dec 18, 2019 | radhika
Environmental cost of sugar
Sep 25, 2019 | radhika
Giving up not an option for women farmers
Dec 18, 2019 | radhika
Workers in sugarcane farms of Uttar Pradesh get a bitter deal
Sep 25, 2019 | radhika
5 takeaways from Study on Sustainability in Sugar Value Chains
Sep 25, 2019 | radhika
Code on Wages lacks clear policy outcome
Nov 21, 2019 | radhika
Caste, Class and Education
Sep 19, 2019 | radhika
Trailblazing on the Path to Education4All
Dec 5, 2019 | radhika
Background Note: State Convention on Proposed Amendments to Indian Forest Act 1927
Feb 20, 2020 | radhika
Recommendations on proposed amendments to the Indian Forest Act 1927
Dec 18, 2019 | radhika
Oxfam India’s Response to Natural Disasters
Dec 5, 2019 | Anisha
Celebrating Women Humanitarians | World Humanitarian Day 2019
Aug 19, 2019 | radhika
जारी है ऐतिहासिक अन्याय
Dec 18, 2019 | radhika
Life at Oxfam India
Dec 18, 2019 | radhika
Why should you make Humanitarian donations to an NGO?
Dec 5, 2019 | radhika
The scourge of manual scavenging
Dec 5, 2019 | radhika
Trailwalker- the ultimate walkathon for a social cause
Dec 18, 2019 | radhika
Making Communities Resilient in Flood-Prone Bihar
Dec 18, 2019 | Anisha
Obligations & choices- the unceasing dilemma
Dec 5, 2019 | radhika
Course on Business and Human Rights – 3rd Edition
Aug 1, 2019 | radhika
जंगल की कविताएं
Jul 31, 2019 | radhika
It is not your job | Unpaid care work in India
Dec 5, 2019 | radhika
Rural healthcare in India — a boon or bane?
Dec 18, 2019 | radhika
For the Gonds, Forest is Heaven on Earth
Dec 5, 2019 | radhika
The Case of Incomplete CFR Titles of Arjuni Village
Dec 5, 2019 | radhika
Oxfam India stands with flood-affected families in Assam
Dec 5, 2019 | Anisha
Undo Historical Injustice to Forest Dwellers, Once Again
Dec 5, 2019 | radhika
Empowering women, one step at a time
Dec 18, 2019 | radhika
Encephalitis is ending our future- our children
Dec 5, 2019 | radhika
#YesDemocracy | Creating fearless spaces for all
Jun 27, 2019 | radhika
Oxfam India collaborates with Josh Talks
Jun 19, 2019 | radhika
Oxfam India pushes for proper implementation of FRA in Chhattisgarh
Dec 18, 2019 | Anisha
Oxfam India’s Community Leader Wins Woman Exemplar Award 2019
Sep 27, 2019 | Anisha
Rebuilding cyclone-affected lives in Odisha
Jun 19, 2019 | Anisha
Marginalised communities in UP fight for their right to healthcare
Dec 18, 2019 | Anisha
Women’s Health on the Backburner in Bihar’s Poll
May 27, 2019 | sanya
Vote for a New India! #YesDemocracy
May 24, 2019 | Anisha
Oxfam India thinks out-of-the-box to restore wells in Kerala
Jul 23, 2020 | ursila
Oxfam’s Learning Lab on Private Sector Engagement
Sep 9, 2019 | ursila
Help Meena break the endless cycle of poverty through education
Sep 9, 2019 | Anisha
Rampant discrimination at Public Health Facilities- Aarti's story
Sep 9, 2019 | ursila
“The IT girl” – Breaking the stereotype of women in tech
May 13, 2019 | ursila
How Oxfam India touched lives in 2018
Sep 30, 2019 | ursila
Five Charities Working For Women
Sep 19, 2022 | ursila
Oxfam India's latest workshop on 'Threat to media, Fake News & #MeToo'
Sep 10, 2019 | ursila
Everything you must know about Oxfam India's fight against inequality
Oct 24, 2019 | ursila
What does Delhi have to say about India's Inequality Problem?
Oct 7, 2019 | ursila
What is Inequality?
Oct 24, 2019 | ursila
Jalaun's Manual Scavengers- Fighting for Right to Life with Dignity
Feb 20, 2020 | ursila
World Wetlands Day- Is India committed towards wetland conservation?
Nov 11, 2019 | ursila
Collective Action integral to Transboundary Risk Governance
Oct 30, 2019 | ursila
Childcare in India today
Jun 3, 2020 | ursila
Oxfam India takes the fight against inequality to the streets
Nov 18, 2019 | ursila
Five moments from 2018 that emboldened the fight for gender justice
Sep 27, 2019 | ursila
Seven frequently asked questions about Oxfam’s Inequality report
Oct 7, 2019 | ursila
Pratima, a casualty of India's growing inequality
May 31, 2020 | ursila
10 powerful quotes to help you understand the global inequality crisis
Oct 24, 2019 | ursila
Inequality through my lens
Oct 24, 2019 | ursila
Achieving water rights by smashing patriarchy
Oct 24, 2019 | ursila
Chennai's resettlement colony shows a grim picture of Inequality
Oct 24, 2019 | ursila
Art Meets Activism with the Illustrate For Impact Fellowship - Register Now
Apr 5, 2019 | ursila
Oxfam India organized two state level consultations under education program
Nov 18, 2019 | Anisha
Secret Superstar: On fighting domestic violence and finding autonomy
Sep 27, 2019 | ursila
Failed Education Priorities of the Bihar Government
Feb 20, 2020 | ursila
Structural injustice in Sugar Cane Agriculture
Sep 9, 2019 | ursila
Addressing malnutrition during a humanitarian crisis
Oct 7, 2019 | ursila
My first experience of handling a natural disaster
Oct 7, 2019 | ursila
15 Healthcare schemes in India that you must know about
Sep 23, 2019 | ursila
Oxfam India marks "16 Days of Activism"
Oct 24, 2019 | Anisha
This unique search engine aims to tackle energy poverty in rural India
Sep 10, 2019 | ursila
10 things you need to know about the RTE Act #HaqBantaHai
Sep 27, 2019 | admin
Two women human rights defenders on the power of mobilisation
Oct 24, 2019 | ursila
Oxfam India Celebrates Child Rights Week
Oct 31, 2019 | oxfamadmin
10 women-led protests that shook the world in 2018
Oct 7, 2019 | ursila
Achieving the SDGs is impossible without empowering Indian women
Apr 5, 2019 | ursila
Social Norms Simplified
Feb 20, 2020 | admin
Child Labour & Child Rights in India: Myth or Reality
Sep 9, 2019 | ursila
Be a ChangeMaker with Oxfam's latest free course on Campaigning, Advocacy and Community Mobilisation
Apr 5, 2019 | admin
Is India committed to reducing inequality? This report finds out more
Sep 9, 2019 | ursila
Oxfam India introduces a course on Gender & Media
Oct 7, 2019 | admin
Section 377 Scrapped: Supreme Court's Verdict Creates History
Oct 7, 2019 | admin
Why I joined the fight for Gender Equality
Oct 24, 2019 | admin
Who is Reaping the Benefits of India’s High Economic Growth?
Oct 24, 2019 | admin
Oxfam India's stand on allegations of sexual harassment against filmmaker of Balekempa
Apr 5, 2019 | admin
Oxfam India's CEO, Amitabh Behar on India's commitment to reduce inequality
Oct 24, 2019 | admin
Move over 'Sons of the soil': Why you need to know the female farmers that are revolutionizing agriculture in India
Oct 7, 2019 | admin
Oxfam India stands in solidarity with #MeToo movement
Oct 24, 2019 | admin
Road to rebuilding “God’s own country” | Aftermath of Kerala Floods
Apr 5, 2019 | admin
Mystery of Out-of-School-Children in the Indian Education System
Sep 27, 2019 | admin
A school with no roof
Oct 24, 2019 | ursila
Oxfam India helping mothers deliver healthy babies
Apr 5, 2019 | Anisha
How Oxfam India is helping crack gender stereotypes in the Indian Film Industry
Oct 24, 2019 | Anisha
Rhymes and plays unite children on Global Handwashing Day
Sep 27, 2019 | Anisha
Why India's girl child deserves a chance at education
Sep 12, 2022 | admin
Oxfam India reaches to over 15,000 people in Kerala
Apr 5, 2019 | Anisha
Oxfam India responds to sexual misconduct by Oxfam GB staff during Haiti Earthquake response in 2010
Oct 7, 2019 | ursila
Oxfam Stands with Kerala
Oct 1, 2019 | Anisha
Oxfam helped over 25,000 people within three months
Oct 30, 2019 | Anisha
Oxfam India engages with youth on ‘Inequality in Education’
Oct 7, 2019 | Anisha
Four reasons why the Forest Rights Act fails to empower forest-dwelling communities
Oct 7, 2019 | ursila
Stories from the ground: Oxfam India’s response to floods 2018
Oct 24, 2019 | Anisha
North East Floods 2018: Oxfam is responding
Apr 5, 2019 | Anisha
Oxfam India’s champion: Megha
Sep 10, 2019 | Anisha
Stories of Change: Scripting Her Own Fate
Oct 7, 2019 | ursila
In pursuit of justice…
Oct 24, 2019 | ursila
Can we afford to overlook Assam Floods?
Oct 7, 2019 | ursila
Everything you need to know about Oxfam India’s response to Assam Floods 2017
Oct 24, 2019 | ursila
How does Oxfam respond during humanitarian disasters like floods?
Oct 24, 2019 | ursila
Oxfam India responds to North East floods 2018
Oct 30, 2019 |
Stories of Change: Strike back the silence
Oct 7, 2019 | ursila
Oxfam’s campaign on Access to Affordable Essential Medicines
Oct 7, 2019 | Anisha
Oxfam’s training programs saving lives
Oct 7, 2019 | Anisha
Chiligi’s fight for education
Oct 1, 2019 | Anisha
Where there is a Will, there is a Way
Oct 7, 2019 | Anisha
Stories of Change: Fighting against all odds
Sep 27, 2019 | ursila
Stories of Change: Breaking Boundaries at Home
Oct 24, 2019 | ursila
Stories of Change: Rise. Resist. Rebel
Oct 1, 2019 | ursila
Stories of Change: Celebrating our feminist heroes
Nov 14, 2019 | ursila
3 Innovations in Disaster Risk Reduction in India you should know about
Oct 24, 2019 | ursila
Oxfam India Disaster Risk Reduction Program Continues
Oct 1, 2019 | Anisha
Oxfam India Builds Water Solution in Disaster Prone Areas
Oct 24, 2019 | Anisha
A Second Chance at Life
Oct 7, 2019 | Anisha
5 books that will change the way you see the world around you
Oct 7, 2019 | ursila
Meet these 3 Warriors who are Fighting Inequality through Education
Apr 5, 2019 | ursila
Meet these 3 Warriors who are Fighting Inequality through Education
Nov 18, 2019 | Anisha
Oxfam India’s innovation building resilient communities.
Sep 9, 2019 | Anisha
Is ineffective healthcare system affecting lives?
Sep 10, 2019 | Anisha
Breaking the shackles of domestic violence
Nov 21, 2019 | Anisha
Listening To The Unheard Voices Of India
Oct 7, 2019 | Anisha
Empower Women, Empower Nation- Oxfam India on International Women’s day
Sep 10, 2019 | Anisha
Yet another International Women’s Day, Yet another Struggle
Sep 27, 2019 | ursila
15 shocking facts about inequality in India
Oct 24, 2019 | ursila
NGOs Strengthening the Education System in India
Sep 20, 2022 | Anisha
Oxfam India’s Humanitarian Champions
Nov 11, 2019 | Anisha
Changing Social Norms Through Education
Oct 7, 2019 | Anisha
The Power of Courage
Oct 24, 2019 | Anisha
Healthcare Awareness Saves Lives
Oct 1, 2019 | Anisha
A World Free From Violence Against Women
Sep 10, 2019 | Anisha
BRIDGING THE GAP
Oct 24, 2019 | Anisha
DISABLING THE DISABILITY
Oct 30, 2019 | Anisha
Children are paying the price of Tax Robbery. Help Stop This. Give A Missed Call on 70977 70977
Oct 1, 2019 | ursila
India’s children are paying the price of Tax Robbery
Oct 24, 2019 | ursila
Reel & Real: Blurred Lines between Cinema and Reality- Notes from Women In Films brunch at Jio MAMI Film Festival
Oct 30, 2019 | ursila
Oxfam Gave Relief to Over 82,000 Lives
Oct 30, 2019 | Anisha
Picture Abhi Baqi Hai, Behena
Oct 1, 2019 | ursila
Assam Drowns Again
Sep 27, 2019 | Anisha
A Long Road Home
Oct 7, 2019 | Anisha
Oxfam India’s letter to President of India requesting affirmative action on passing Women’s Reservation Bill in Parliament.
Sep 10, 2019 | oxfamadmin
Women Representation in Political Decision Making: A Catalyst to achieving Gender Equality
Oct 24, 2019 | ursila
Will Fear of ‘Failing’ Make India Literate?
Sep 27, 2019 | ursila
WATER IS LIFE
Nov 18, 2019 | Anisha
Building bridges: The journey of a teacher par excellence
Oct 7, 2019 | ursila
Examining humanitarian aid through the gender lens
Oct 24, 2019 | ursila
The pathways to gender equality are far from straight
Oct 7, 2019 | ursila
The changing world of humanitarian work
Sep 10, 2019 | ursila
Can India be a Leader in Disaster Risk Reduction Measures in Asia?
Oct 7, 2019 | ursila
A struggle for survival: Assam Floods
Nov 11, 2019 | Anisha
Lessons to be learnt from the Gorakhpur tragedy
Oct 24, 2019 | ursila
Is Section 498A anti women?
Nov 11, 2019 | ursila
The Irresistible & Oppressive Gaze: A Survey Report by Oxfam India
Oct 24, 2019 | oxfamadmin
North East Floods: How you can help those affected?
Oct 1, 2019 | Ravi
Oxfam is responding in Assam Floods 2017
Oct 1, 2019 | Ravi
Lipstick Under My Burkha Official Trailer - Winner of Oxfam's Best Film on Gender Equality Award
Sep 27, 2019 | Ravi
Sourcing Life
Oct 7, 2019 | Anisha
MEETING TOILET TARGETS
Oct 7, 2019 | oxfamadmin
Disaster Changed Her Life
Oct 24, 2019 | Anisha
#HaqBantaHai Campaign on Access to Free Medicine: Bihar
Sep 10, 2019 | Anisha
Be The New Norm
Oct 7, 2019 | Ravi
Oxfam India’s Recommendations for National Policy for Women
Sep 27, 2019 | Ravi
The Greatest Earning: EDUCATION
Dec 5, 2019 | Anisha
Women Farmers or Labourers?
Oct 24, 2019 | Avantika
Farewell Dirty Water
Jan 9, 2020 | Avantika
Clean Water Can Save Lives
Oct 24, 2019 | Avantika
Making men an ally on women's rights
Oct 24, 2019 | Avantika
'Initially the men opposed. They thought we women were being disruptive.'
Oct 1, 2019 | Avantika
Tax havens resist reforms one year on from Panama Papers exposé
Oct 1, 2019 | Avantika
इख़्तियार
Oct 24, 2019 | Avantika
Lessons from the Grassroots
Sep 10, 2019 | Avantika
This is What Child Marriage Looks Like
Nov 18, 2019 | Avantika
Oxfam India Held Youth Festivals In Lucknow And Raipur
Sep 9, 2019 | Avantika
Oxfam at the North-East Disaster Risk Reduction Conclave 2017
Sep 9, 2019 | Avantika
Finding Solutions to Early and Forced Marriage
Sep 27, 2019 | Avantika
Silence Has No Honour
Sep 27, 2019 | Avantika
Solidarity Is Our Weapon- The International Women’s Strike
Oct 24, 2019 | Avantika
4 reasons why Oxfam supports the International Women’s Strike on the 8th March
Oct 24, 2019 | Avantika
Union Budget 2017-18: Neglected Social Sector
Sep 10, 2019 | Avantika
Putting Data at the Heart of Business Responsibility
May 13, 2019 | Avantika
Mainstreaming DRR in Local Development Plans to Reduce Aid Dependency
Oct 1, 2019 | Avantika
Union Budget 2017-18: A Look at the Health Sector
Apr 5, 2019 | Avantika
खेल - जेण्डर आधारित असमानताओं को उजागर करने को एक सषक्त माध्यम
Apr 5, 2019 | oxfamadmin
Why Brazil should not take a U-turn on its health system
Oct 7, 2019 | Avantika
Your questions answered: Oxfam’s Inequality report
Oct 1, 2019 | Avantika
Unpacking the Risks of Doing Business in India
Nov 14, 2019 | Avantika
We Never Learn
Sep 27, 2019 | Ravi
Promote men’s involvement for changing social norms
Oct 24, 2019 | Avantika
Ten years of the Forest Rights Act: Opportunity lost?
Oct 1, 2019 | oxfamadmin
Meet the Bravehearts Standing Up Against Domestic Violence
May 27, 2020 | oxfamadmin
Addressing Violence Against Women and Girls the SAARC Way: Combat Human Trafficking
Sep 10, 2019 | oxfamadmin
Oxfam India’s journey from programme to campaign
Oct 24, 2019 | oxfamadmin
सामाजिक मान्यताओं को चुनौती देता संगठन
Dec 5, 2019 | oxfamadmin
Changing The World – One Couple At A Time
Oct 24, 2019 | oxfamadmin
A Lesson on Education from Uttar Pradesh
Oct 7, 2019 | oxfamadmin
Fair Sharing of Mining Revenue for the Tribals
Oct 24, 2019 | oxfamadmin
An Open Letter to Chhotu, Munna and Bachcha
Jun 12, 2020 | oxfamadmin
Educating the Educators
Sep 27, 2019 | oxfamadmin
10 Years of Domestic Violence Act: The Way Ahead
Oct 24, 2019 | oxfamadmin
Oxfam Best Film on Gender Equality Award Gets Grand Reception
Sep 27, 2019 | oxfamadmin
Wrestling Social Norms Out
Oct 3, 2019 | oxfamadmin
The Toilet Conundrum
Oct 24, 2019 | oxfamadmin
Inequality in India: what's the real story?
Sep 27, 2019 | oxfamadmin
Making surface water safe for drinking
Oct 1, 2019 | oxfamadmin
Quality Education- The unfinished agenda of RTE Act
Sep 27, 2019 | oxfamadmin
Tale of Two Women
Sep 27, 2019 | oxfamadmin
Prioritising the Health of our Children
Oct 24, 2019 | oxfamadmin
Violence in women’s own backyard
Sep 9, 2019 | oxfamadmin
We failed yet again
Sep 10, 2019 | oxfamadmin
Providing access to iron-free drinking water
Oct 7, 2019 | oxfamadmin
Her Series - Tale of Buguru Chitamma: How a cooperative transformed fisher women into leaders
Oct 24, 2019 | oxfamadmin
Why the CAF bill conflicts with the Forest Rights Act?
Oct 7, 2019 | oxfamadmin
Renew to Live Anew
Sep 9, 2019 | oxfamadmin
What do we want: Health as a ‘Right’ or just an ‘Assurance’
Nov 18, 2019 | oxfamadmin
Oxfam International signs historic deal to move to Nairobi, Kenya
Oct 24, 2019 | oxfamadmin
Why is passing the Women’s Reservation Bill urgent?
Sep 19, 2023 | oxfamadmin
BREXIT & What It Means for Humanitarian Aid
Oct 7, 2019 | oxfamadmin
Rahul Bose: Films should be gender sensitive
Oct 24, 2019 | oxfamadmin
Portrait of a Teacher: Successful introduction of multi-lingual education for Odisha’s tribal communities
Nov 6, 2019 | oxfamadmin
Tax dodging is a crime against developing countries
Sep 10, 2019 | oxfamadmin
Signs of social risks impacting Indian businesses
Oct 7, 2019 | oxfamadmin
Tikamgarh revisited, what’s happened to the amazing fishing communities I visited in 2006?
Jan 9, 2020 | oxfamadmin
Where school means freedom
Sep 10, 2019 | oxfamadmin
Yes, Prime Minister
Oct 30, 2019 | oxfamadmin
India’s National Budget 2016-17: Missed Opportunity to Address Inequality?
Oct 1, 2019 | oxfamadmin
Free The Night
Sep 9, 2019 | oxfamadmin
Woman, Open Your Eyes…
Oct 24, 2019 | oxfamadmin
From Darbhanga to Davos: Access to Affordable Medicine Still Remains a Key Question
Dec 16, 2019 | oxfamadmin
Hoping for a Second Chance: Punita Devi
Sep 27, 2019 | oxfamadmin
Activating Youth in Lucknow to Promote Girls’ Education
Sep 27, 2019 | oxfamadmin
Change is Coming: Rani Bitti’s Story
Sep 10, 2019 | oxfamadmin
Rachna’s Fight for Justice
Oct 7, 2019 | oxfamadmin
3 Key Observations from #WEF2016 that Indian Businesses Must Take Note Of
Sep 27, 2019 | oxfamadmin
Here’s Why States Need to Provide Free Basic Medicines
Nov 18, 2019 | oxfamadmin
Update: Oxfam to Provide Shelter to 300 Households Hit by The Manipur Earthquake
Apr 5, 2019 | oxfamadmin
In El Salvador, a struggle to survive El Niño
Oct 24, 2019 | oxfamadmin
Bihar designs a 15-year roadmap to reduce risk of disaster
Feb 20, 2020 | ursila
Violence as an Effective Mode of “Indian” Communication
Apr 5, 2019 | oxfamadmin
Because it’s 2015!
Sep 27, 2019 | oxfamadmin
Let’s welcome a new dawn, minus domestic violence
Oct 24, 2019 | oxfamadmin
Data and Discrimination: Women’s Ownership of Assets in India
Oct 24, 2019 | oxfamadmin
“No Woman, No Cry!”
Sep 27, 2019 | oxfamadmin
Pushing, pulling and the power of people: new horizons for corporate responsibility?
Jan 9, 2020 | oxfamadmin
Yes bank - say to inclusive and social banking and inclusive business model
Sep 27, 2019 | oxfamadmin
Creating shared value through inclusive business
Oct 7, 2019 | oxfamadmin
TATA consultancy services – empowering farmers with mobile technology
Sep 27, 2019 | oxfamadmin
What the CSR numbers don’t tell
Oct 1, 2019 | oxfamadmin
6 important things companies need to do to be inclusive
Nov 21, 2019 | oxfamadmin
Why businesses need to invest in creating a productive population for a sustainable future
Sep 10, 2019 | oxfamadmin
Jaipur rugs – weaving the lives of the poor into the global markets. an inclusive business model.
Oct 24, 2019 | oxfamadmin
The next 15 years: highlighting the role of the private sector in development
Oct 7, 2019 | oxfamadmin
Emphasizing a human rights-based approach to inclusiveness in business
Oct 30, 2019 | oxfamadmin
Privatising Forests: A Bad Idea
Oct 30, 2019 | oxfamadmin
Adoption of Agenda 2030: 17 SDGs for 15 years
Nov 15, 2019 | oxfamadmin
Five questions about the #GlobalGoals you were too embarrassed to ask
Oct 7, 2019 | oxfamadmin
Last mile smile
Oct 7, 2019 | oxfamadmin
Social responsibility of companies should not stop at 2%
Sep 27, 2019 | oxfamadmin
In ‘campaign mode’, states flout FRA rules
Sep 27, 2019 | oxfamadmin
“I will not leave my forest. I will keep my jungle”
Oct 1, 2019 | oxfamadmin
Where is the nutrition? Ask pregnant women in a village of Bihar
Jan 9, 2020 | oxfamadmin
Learning to read at schools, but where are the textbooks?
Oct 24, 2019 | oxfamadmin
Progressive tax norms must underlie financing of the Sustainable Development Goals
Sep 27, 2019 | oxfamadmin
Teachers needed! Government schools are falling behind due to lack of funds
Oct 24, 2019 | oxfamadmin
Protect and expand India’s public healthcare system: The inequality imperative
Dec 16, 2019 | oxfamadmin
“On My Second Day At School, A Kid Asked Me What Caste I Was”
Oct 7, 2019 | oxfamadmin
India’s missing girls: A tale of healthcare neglect faced by girls
Sep 9, 2019 | oxfamadmin
Should we only give attention to women’s health on International day of action?
Nov 18, 2019 | oxfamadmin
No respite for 72-year-old Sitaram, a month after #NepalEarthquake
Oct 7, 2019 | oxfamadmin
One month on, education of children still jolted by Nepal earthquake
Oct 24, 2019 | oxfamadmin
New worry for Nepal; landslides, floods may block relief work
Oct 7, 2019 | oxfamadmin
Monsoon preview in Kathmandu blows away shelters in relief camp
Oct 1, 2019 | oxfamadmin
Last mile distribution of relief supplies is biggest challenge in Nepal: Indian ambassador
Oct 7, 2019 | oxfamadmin
When Delhi’s Streets Buzzed with ‘Haq Banta Hai’
Oct 7, 2019 | oxfamadmin
Lack of water, toilets making things worse for women in Nepal
Oct 7, 2019 | oxfamadmin
Oxfam India gets government approval to respond to #NepalEarthquake in 28 hours
Apr 5, 2019 | oxfamadmin
Desperation creeping in, people in Nepal wait for aid
Oct 7, 2019 | oxfamadmin
#OxfaminNepal: “More than 60,000 litres of water has been provided till now”
Oct 7, 2019 | Avantika
Political (and some other) priorities in Nepal as of 28 April 2015
Oct 30, 2019 | oxfamadmin
#Nepal Earthquake: “The death toll has crossed 2000 and this is just the beginning”
Jan 9, 2020 | oxfamadmin
#NepalEarthquake: It is going to be a long road to recovery
Oct 24, 2019 | oxfamadmin
Money Matters!
Oct 24, 2019 | oxfamadmin
All for Education, Education for All
Oct 7, 2019 | oxfamadmin
When schools continue to exclude, can education reduce caste discrimination in India?
Feb 20, 2020 | oxfamadmin
Ensuring the right to education, forming bonds for life
Oct 1, 2019 | oxfamadmin
How can India send a spaceship to Mars but not educate its children?
Sep 30, 2019 | oxfamadmin
India wins in cricket, but losing out on education
Sep 30, 2019 | oxfamadmin
Oxfam's 'Even it up' report a must read lesson on Inequality
Oct 24, 2019 | oxfamadmin
It’s time to understand ‘womanhood is beyond maternity’
Oct 7, 2019 | oxfamadmin
The True Measure of Land's Value
Oct 7, 2019 | oxfamadmin
The “Ten-thousand Committee”: Reviving VHSNCs in Jharkhand
Oct 1, 2019 | oxfamadmin
Singing their way out of child marriage
Sep 10, 2019 | oxfamadmin
Land Acquisition bill tests government’s pro-poor stance
Oct 1, 2019 | oxfamadmin
Breaking the silence, standing tall
Sep 27, 2019 | oxfamadmin
Making a Song and Dance about Child Marriage
Oct 7, 2019 | oxfamadmin
Let’s Talk About Sex
Sep 10, 2019 | oxfamadmin
Mobile technology solutions could be a game changer for maternal health: Scribes
Sep 27, 2019 | oxfamadmin
Missing Girls: The Puzzling Domestic Violence Agenda
Oct 3, 2019 | oxfamadmin
Her Ghar: A right to residence for every woman
Oct 7, 2019 | oxfamadmin
Considering Gender: A Mediaperson’s Guide to Covering Disasters
Dec 16, 2019 | oxfamadmin
True Grit
Apr 5, 2019 | oxfamadmin
Violence against women and star power: Does their magic wand work?
Oct 24, 2019 | oxfamadmin
Having Those Difficult Conversations
Oct 24, 2019 | oxfamadmin
Day of the Man: guarding the china shop
Oct 7, 2019 | oxfamadmin
Gender parity needs to begin at home with mother’s guardianship rights!
Sep 9, 2019 | oxfamadmin
It’s a Girl!
Oct 1, 2019 | oxfamadmin
Let’s Help End Domestic Violence!
Oct 24, 2019 | oxfamadmin
A Few Good Men
Oct 7, 2019 | oxfamadmin
Promises to keep—Implementation of PWDV Act in Odisha
Sep 27, 2019 | oxfamadmin
Make 16 Days of Activism an Everyday Practice
Oct 30, 2019 | oxfamadmin
Witch-Hunting: A less talked about form of Violence Against Women
Oct 24, 2019 | oxfamadmin
Markets Also Discriminate
Oct 7, 2019 | oxfamadmin
Let’s Talk About Domestic Violence!
Oct 7, 2019 | oxfamadmin
Getting Serious about Ending Violence against Women and Girls
Oct 3, 2019 | oxfamadmin
Right to a Violence Free Life
Sep 10, 2019 | oxfamadmin
It’s all about the money
Sep 10, 2019 | oxfamadmin
‘It’s No Longer Funny': The Funding Wars That’ll Dictate Our Future
Oct 7, 2019 | oxfamadmin
Girl, Interrupted
Oct 1, 2019 | oxfamadmin
16 Pictures From Imagining Inequality That WiIl Tell You The Truth #evenitup
Oct 24, 2019 | oxfamadmin
These 8 Goals Were Set To Develop The World, But 14 Years Since, This Is Where We Stand
Dec 5, 2019 |
A Look At The Year 2029: What Kind Of Legacy Will We Leave Behind For Our Future Generations?
Nov 18, 2019 |
These 8 Goals Were Set To Develop The World, But 14 Years Since, This Is Where We Stand
Oct 24, 2019 | oxfamadmin
BRICS bank a necessary step, but needs more transparency
Sep 9, 2019 |
Short term memory and Long term needs!
Oct 7, 2019 |
A people’s budget has to go beyond...
Oct 24, 2019 |
National Shame, National Failure
Sep 27, 2019 | oxfamadmin
Oxfam India pledges its support to #BringBackOurGirls
Oct 1, 2019 | oxfamadmin
Closing the Gap on Gender: Is India up for the challenge?
Nov 15, 2019 | oxfamadmin
She tills, she sows, but she does not own
Oct 7, 2019 | oxfamadmin
Take a pause: what do the Uttrakhand floods tell us about India’s development model?
Sep 10, 2019 | oxfamadmin
Saving lives on sharp turning roads
Oct 1, 2019 | oxfamadmin
They do mind the gap
Oct 7, 2019 | oxfamadmin
Right to Education, still a long way to go.
Oct 1, 2019 | oxfamadmin
Can We Close the Gap on Women's Inequality in India?
Oct 30, 2019 | oxfamadmin
Breaking Old Barriers and Building New Alliances for Food Justice in India and Globally
Oct 24, 2019 | oxfamadmin